Abstract
Objectives: The purpose of this study was to investigate the relationship between mental healthlevel,usual lifestyle, and thelevelofsubjectivesymptoms of some adults. Methods: From 17 September—28 November 2017, 260 adults living in Seoul, Gyeonggi, and Incheon completedaquestionnaireconsistingofgeneral characteristics (6 items), mental health level (14 items), usual lifestyle (9 items), and subjective symptoms level (9 items) on a 5-point scale. Results: In the mental health level, there was a significant difference in sex, age, marital status, education level, andexistenceofstress, and there were differences in age, marital status, occupation, and existence of stress in usual lifestyle. There were statistically significant differences in age, marital status, occupation, and existenceofstress in the subjective symptoms of temporomandibular disorders. Conclusions: It is necessary to develop a program that can be applied in parallel with counseling therapy related to mental health during the clinical treatment of temporomandibular disorders.
Figures & Tables
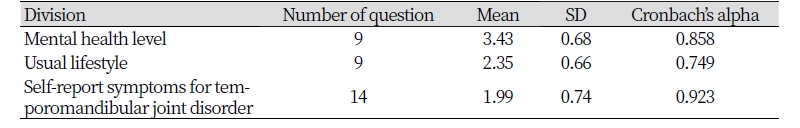
Table 1. Subject’s mental health level, usual lifestyle and self-report symptoms for temporomandibular joint disorders (N=260)


