Abstract
Objectives: The study aimed to isolate the abundant bacteria in dental caries in children and to investigate the bacterial species involved in addition to those that have been previously reported. Methods: The specimens were collected from the supragingival plaques of each dental caries area, pit and fissure caries, deep dentinal caries, smooth surface caries, and dental caries, and from healthy subjects in the control group. Bacteria were cultured from these specimens, DNA was extracted from the isolated bacteria, and the 16S rRNA gene sequences were analyzed and identified. Results: Based on the results of the 16S rRNA gene sequence analysis for the 90 strains of dominant bacteria from the 45 specimens, 5, 7, 8, 7, and 13 species were identified from the supragingival plaques from healthy teeth, pit and fissure caries, deep dentinal caries, smooth surface caries, and dental caries, respectively. In healthy teeth, Actinomyces naeslundii dominated. Corynebacterium durum, Ralstonia pickettii, and Streptococcus intermedius showed equal distribution. The dominant bacterial species in dental caries, S. sanguinis, showed the greatest difference in prevalence in pit and fissure caries. In deep dentinal caries, S. mutans and Lactobacillus rhamnosus were dominant; in smooth surface caries, S. mutans and S. sanguinis were dominant; and in the supragingival plaques of dental caries, S. sanguinis and S. mutans were dominant. Conclusions: The bacterial species isolated from dental caries encompassed four phyla, eight genera, and 22 species. In addition, the SS1-2 strain, belonging to the genus Neisseria, was identified as a new species from among the isolated strains.
Figures & Tables
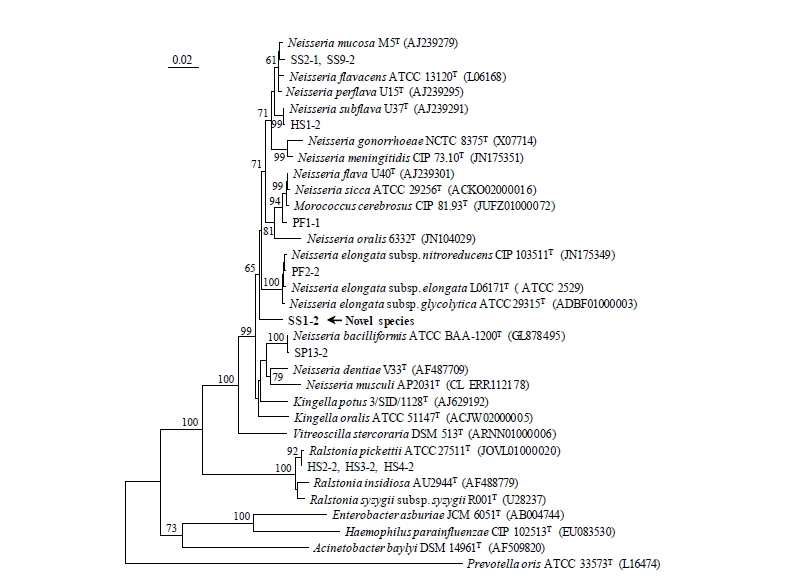
Fig. 1. Neighbour-joining tree based on partial 16S rRNA gene sequences showing relationships between dental caries and related genera of the phylum Proteobacteria. The percentage numbers at the nodes indicate the bootstrap support levels, based on neighbor-joining analysis of 1,000 resampled data sets. Bar, 0.02 nucleotide changes per 16S rRNA gene position. HS, healthy subject; PF, pit and fissure caries; SS, smooth surface caries; SP, supragingival plaque


