1Department of Oral Health Sciences, School of Health Sciences, Meikai University
2Department of Pediatric Dentistry・Special Needs Dentistry, Institute of Science Tokyo
Correspondence to Yu-Jeong Shin, Department of Oral Health Sciences, School of Health Sciences, Meikai University, Akemi 1, Urayasu, Chiba 279-8550, Japan. Tel: +81-47-355-5111, E-mail: shin.y.8de1@m.isct.ac.jp
Volume 25, Number 6, Pages 465-71, December 2025.
J Korean Soc Dent Hyg 2025;25(6):465-71. https://doi.org/10.13065/jksdh.2025.25.6.1
Received on December 11, 2025, Revised on December 15, 2025, Accepted on December 17, 2025, Published on December 30, 2025.
Copyright © 2025 Journal of Korean Society of Dental Hygiene.
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License(http://creativecommons.org/licenses/by-nc/4.0).
Objectives: Japan’s rapid transition into a super-aging society has reshaped oral health needs and dental hygiene education. This study aims to examine the evolution of Japan’s gerodontology and dental hygiene education within the context of long-term care reforms and expanding professional roles. Methods: A literature-based review was conducted by synthesizing national policies, legal regulations, and educational guidelines to analyze structural changes in gerodontology education. Results: Policy reforms, particularly the establishment and revision of the long-term care Insurance system accelerated. Educational reforms followed these systemic changes, culminating in the 2022 Educational Principles of Dental Hygienist in Gerodontology. However, persistent challenges remain, including limited clinical training sites, shortages of qualified instructors, inconsistencies in practicum content, and insufficient interprofessional education. Conclusions: Japan’s experience demonstrate the importance of aligning gerodontology education. These findings suggest that Korea would benefit from standardized, competency-based gerodontology curriculum to better prepare practitioner for an aging society.
Dental hygiene education, Dental hygienist, Gerodontology, Japanese dental education
Japan has undergone an exceptional demographic transition characterized by rapid and continuous population aging. While adults aged 65 years and older were less than 5% of the population in 1950, this figure surpassed 14% by 1994, officially classifying the country as an ‘aged society.’ As of 2024, older adults constitute approximately 29.3% of the national population, with those aged 65-74 accounting for 12.5% and those aged 75 and older for 16.8% of the population [1]. Consequently, Japan is widely recognized as the world’s earliest and most advanced ‘super-aging society.’
Such demographic changes have profoundly altered healthcare demands, including those related to oral health. Aging is commonly accompanied by progressive impairment in oral function, including decreased chewing efficiency, compromised swallowing ability, reduced salivary secretion, and an increased prevalence of chronic systemic conditions. These physiological changes heighten the risks of aspiration pneumonia, malnutrition, frailty, and deterioration in overall quality of life (QOL) [2], positioning the maintenance and promotion of oral function as a core component of comprehensive geriatric care.
The diversification of oral health needs has simultaneously reshaped the professional responsibilities of dental hygienists. Traditionally, dental hygiene education emphasized chairside assistance and basic preventive procedures. However, this training model no longer aligns with the increasingly complex needs of older adults. The demographic and social transformation described above consequently motivated a systematic restructuring of dental hygiene education in Japan, particularly the integration of gerodontology into the formal curriculum.
In response to these demographic and clinical shifts, Japan has undertaken systematic reforms in dental hygiene education, including the formal integration of gerodontology into national curricula. However, comprehensive analyses linking population aging policy-driven role expansion, and educational reform remain limited. This review addresses by examining gerodontology education for dental hygienists in Japan.
A major policy shift occurred with the establishment of the Long-Term Care Insurance (LTCI) system in 2000 [3], which initially aimed to provide compensatory care for older adults requiring support. <Fig. 1> presents the ‘Flow of procedures pertaining to use of long-term care service,’ summarizing the steps from initial assessment to service provision. However, rapidly increasing longterm care expenditures soon prompted a series of reforms. In 2005, the LTCI Act was revised to prioritize the prevention of functional decline [4]. This policy revision introduced ‘new preventive benefits’ and a network of community-based support services intended to identify older adults at risk of needing long-term care and to implement early, structured preventive interventions.
Within this framework, ‘oral function improvement services’ were explicitly included as one of the major preventive programs, alongside nutritional and physical function interventions [5]. This marked an important shift in national healthcare policy, as oral health was officially acknowledged as integral to sustaining independence and preventing disability in later life.
Subsequent revisions strengthened this preventive orientation. In 2006, reforms to the medical insurance system increased costsharing for older adults, and in 2018, the Late-Stage Elderly Medical Care System was launched as a dedicated scheme for individuals aged 75 years or older [6].
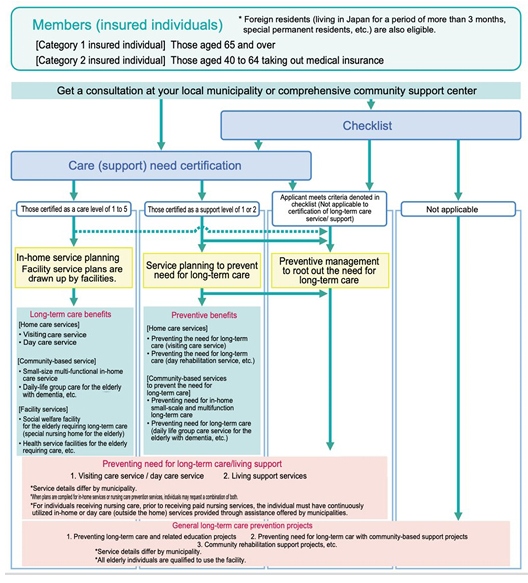
Fig. 1. Flow of procedures pertaining to use of long-term care service; source by [7]
Collectively, these policy reforms reflected a broader shift in Japan’s healthcare system toward prevention-oriented and functioncentered care for older adults, providing an institutional foundation for integration of oral health into long-term care.
Corresponding to these systemic shifts, the legally defined scope of practice for dental hygienists has expanded progressively. Historically, dental hygienists were engaged primarily in preventive services related to caries and periodontal disease, oral hygiene instruction, and clinical assistance during dental treatment [8].
As the significance of oral function in geriatric health became widely recognized, dental hygienists began to assume broader responsibilities, including assessment of oral and swallowing functions, participation in aspiration pneumonia prevention, provision of oral and swallowing rehabilitation, and collaboration within multidisciplinary care teams involving physicians, nurses, dietitians, and care works [8,9].
Additionally, reimbursement policies were amended in 2019 [10] to introduce additional incentives related to oral function maintenance, nutrition monitoring, and other facility-based oral health management services. These changes helped formalize the role of dental hygienists as essential contributor to preventive and rehabilitation geriatric care rather than solely clinical assistants.
This evolution of professional responsibilities illustrates how policy and reimbursement changes were closely aligned with the growing recognition of oral function as a component of geriatric health management.
Transformation in clinical practice necessitated corresponding reforms in educational programs, underscoring the need for a systemic educational response to population aging and expanded professional roles. For many years, Japan lacked national-level guidelines for geriatric dentistry education [10]. However, the demographic shift toward an older population and the growing complexity of oral health needs led to increasing calls for structured gerodontology training [11].
In 2009, the Japanese Society of Gerodontology articulated key changes in the clinical landscape through its published ‘goals of gerodontology.’ In 2015, the Society issued the first set of ‘educational principles of gerodontology’ [12], making a critical step toward standardizing geriatric content across dental curricula. The following year, a nationwide survey of 29 dental schools was conducted to assess the implementation status of gerodontology education [13].
Efforts extended to dental hygiene education in subsequent years. A 2018 national survey examining gerodontology education for dental hygienist programs identified persistent barriers, including limited faculty expertise, insufficient instructional hours, and inadequate teaching materials [14]. These findings highlighted the necessity of establishing an evidence-based and unified educational framework.
In response, the ‘Educational Principles of Dental Hygienist in Gerodontology’ was issued in 2022 <Fig. 2> [15]. The document emphasized that dental hygienists working in a super-aging society must be competent not only in clinical dental care but also in home-based care, hospital settings, and long-term care facilities. The curriculum was expanded to include a comprehensive set of topics such as dysphagia, systemic diseases common among older status, behavioral and psychological aspects of aging, caregiving principles, and relevant healthcare laws.
Taken together, these educational developments demonstrate a gradual but systematic effort to align dental hygiene education with policy reforms and the evolving clinical demands of a super-aging society.
The core competence outlined in the 2022 guidelines includes: (1) foundational knowledge required for providing oral healthcare to older adults with or without systemic diseases; (2) competencies related to domiciliary dental care; (3) clinical abilities necessary for delivering care in hospital and home-based settings; (4) understanding of systemic diseases and the pharmacological factors that influence dental treatment; and (5) basic knowledge and practical skills in eating and swallowing rehabilitation.
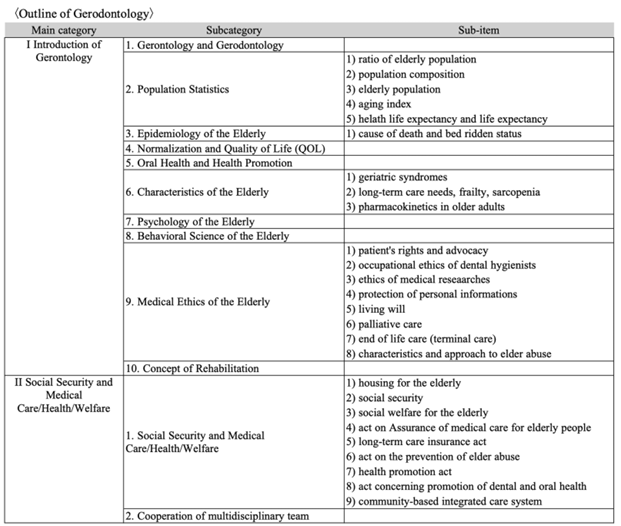
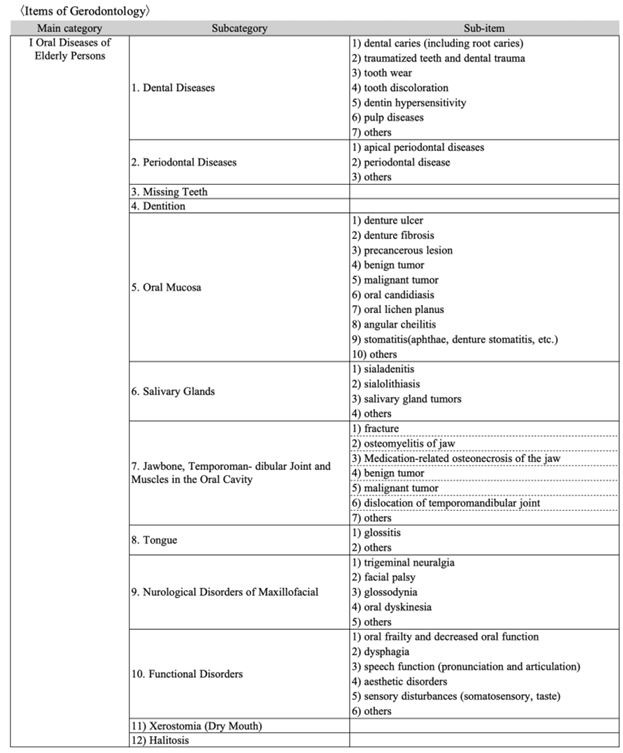
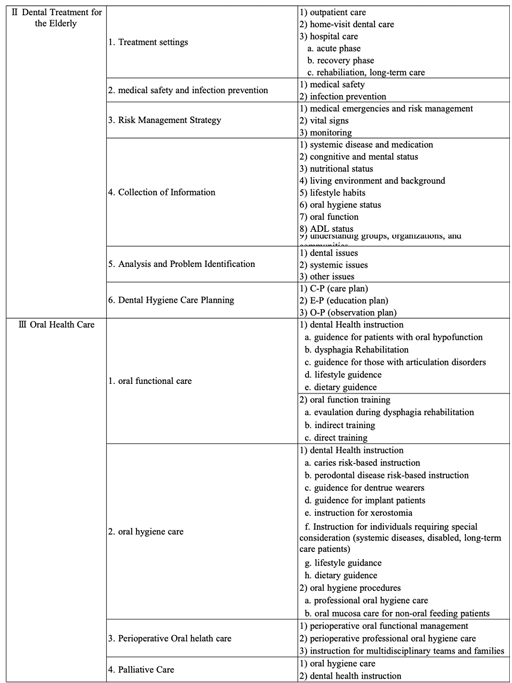
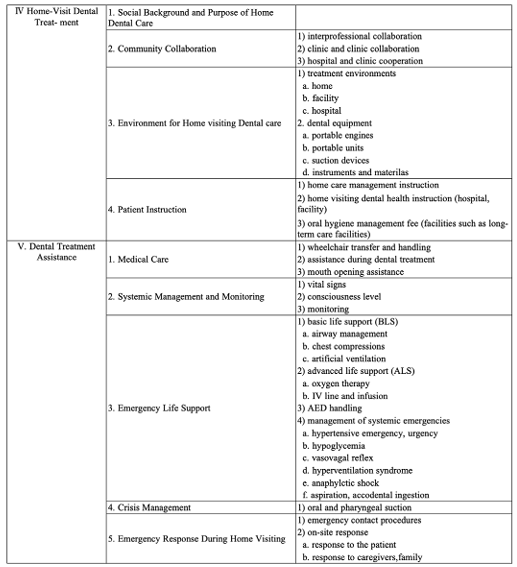
Fig. 2. Educational Principles of Dental Hygienist in gerodontology; source by [15]
This study contributes to the literature by systematically examining how long-term care policy reforms and legal expansions of professional roles have shaped the development of gerodontology education for dental hygienists in Japan.
Although Japan has modernized its dental hygiene curriculum over the past several decades, substantial gaps remain in the practical implementation of gerodontology education, including variability in instructional hours, limited availability of clinical training sites, inconsistencies in practicum quality, shortages of experienced instructors, and insufficient interprofessional learning opportunities [13]. To compensate for these constraints, some programs have incorporated simulation-based teaching methods, including visual case materials, geriatric experience suits, and swallowing-function simulators [16]. These findings collectively highlight the need to strengthen both the educational infrastructure and instructional strategies for gerodontology within dental hygiene programs.
As Japan experiences rapid population aging–accompanied by declining dental caries prevalence, the needs of dental care are undergoing significant transformation. Consequently, the scope of practice required of dental hygienists has become increasingly diverse and complex [17].
Japan’s experience provides meaningful implications for Korea, where population aging is progressing even more rapidly. The Japanese model, which includes the legal expansion of dentists’ responsibilities, competency-based gerodontology guidelines, and the incorporation of community-care principles, demonstrates the value of a structured and future-oriented educational framework [15]. For Korea, it is essential to establish standardized gerodontology competencies within dental hygiene curricula. Furthermore, incorporating AI-assisted learning systems, simulation-based instruction, interprofessional modules, and diverse clinical placements, including hospitals, long-term care facilities, and home-visit dentistry, will be critical to ensuring that Korean dental hygienists are prepared to deliver high-quality oral healthcare for the rapidly expanding older population.
The author fully participated in the work performed and documented truthfully.
YJ Shin is a member of the Editorial Committee of the Journal of the Korean Society of Dental Hygiene, but was not involved in the review process of this manuscript. The authors declare no other conflicts of interest.
None.
Non-human or animal research.
Data can be obtained from the corresponding author.
None.
Cabinet Office (Japan). White paper on the ageing society: 2025 edition [Internet]. Tokyo: Cabinet Office; 2025 [cited 2025 Dec 10]. Available from: https://www8.cao.go.jp/kourei/whitepaper/w-2025/zenbun/07pdf_index.html.
Hasegawa Y, Sakuramoto-Sadakane A, Nagai K, Tamaoka J, Oshitani M, Ono T, et al. Does oral hypofunction promote social withdrawal in the older adults? A longitudinal survey of elderly subjects in rural Japan. Int J Environ Res Public Health. 2020;17(23):8904. https://doi.org/10.3390/ijerph17238904.
Yamada M, Arai H. Long-term care system in Japan. Ann Geriatr Med Res. 2020;24(3):174-80. https://doi.org/10.4235/agmr.20.0037.
Tsutsui T, Muramatsu N. Care-needs certification in the long-term care insurance system of Japan. J Am Geriatr Soc. 2005;53(3):522-7. https://doi.org/10.1111/j.1532-5415.2005.53175.x.
Ministry of Health, Labour and Welfare (Japan). Long-term care insurance system of Japan [Internet]. Tokyo: Ministry of Health, Labour and Welfare; 2025 [cited 2025 Dec 10]. Available from: https://www.mhlw.go.jp/english/policy/care-welfare/care-welfare-elderly/dl/ltcisj_e.pdf.
Ishii T. The medical care system for the late-stage elderly and dental health care. Gerodontology. 2008;23(2):83-9. https://doi.org/10.11259/jsg1987.23.83.
Tokyo Metropolitan Government. Long-term care insurance system [Internet]. Tokyo: Tokyo Metropolitan Government; 2024 [cited 2025 Dec 10]. Available from: https://www.fukushi.metro.tokyo.lg.jp/documents/d/fukushi/R6kaigohokenn-Engver.
Ishii T, Maki Y, Hirata S. Developing role of dental hygienists in Japan. Jpn Dent Sci Rev. 2012;48:135-40. https://doi.org/10.1016/j.jdsr.2012.02.005.
Okada A, Nomura Y, Ohara Y, Yamamoto Y, Hosoya N, Hanada N, et al. Factors affecting the reinstatement of the Japanese dental hygienist: A Japanese dental hygienist survey conducted in 2019. Int J Environ Res Public Health. 2021;18(4):2049. https://doi.org/10.3390/ijerph18042049.
Ono S, Ishimaru M, Yamana H, Morita K, Ono Y, Matsui H, et al. Enhanced oral care and health outcomes among nursing facility residents: analysis using the national long-term care database in Japan. J Am Med Dir Assoc. 2017;18(3):277e1-5. https://doi.org/10.1016/j.jamda.2016.11.024.
Kitagawa N, Sato Y, Komabayashi T. Graduate and undergraduate geriatric dentistry education in a selected dental school in Japan. Eur J Dent Educ. 2011;15(4):231–5. https://doi.org/10.1111/j.1600-0579.2010.00664.x.
Japanese Society of Gerodontology. Educational guidelines for gerodontology (2015 edition) [Internet]. Tokyo: Japanese Society of Gerodontology; 2015 [cited 2025 Dec 10]. Available from: https://www.gerodontology.jp/publishing/file/education_standards.pdf.
Ito K, Fukushima M, Kawara M, Sakaguchi H, Owatari T, Ogasawara T, et al. Current status of gerodontology education in dental schools in Japan. Gerodontology. 2017;32(2):65-71. https://doi.org/10.11259/jsg.32.65.
Ito K, Fukushima M, Kawara M, Sakaguchi H, Owatari T, Ogasawara T, et al. Current status of gerodontology education in dental hygienist training schools in Japan. Gerodontology. 2018;32(4):457-67. https://doi.org/10.11259/jsg.32.457.
Mizuguchi S, Ogasawara T, Aida H, Aritomo T, Ito K, Owatari T, et al. Educational guidelines for dental hygienists in gerodontology. Gerodontology. 2022;37(Sl):E1-7. https://doi.org/10.11259/jsg.37.supplement_1.
Iijima Y, Asakawa A, Aiba C. Educational effects of learning programs incorporating simulated aging experiences in dental hygiene education. J Jpn Oral Health Soc. 2020;10(1):81-6. https://doi.org/10.32303/jnohs.10.1_81.
Ministry of Health, Labour and Welfare (Japan). Current status of dental hygienists and future directions for policy discussion [Internet]. Tokyo: Ministry of Health, Labour and Welfare; 2025 [cited 2025 Dec 10]. Available from: https://www.mhlw.go.jp/content/10804000/001363491.pdf.